
Educators in every field of study have had this experience: as they stand before the class ready to impart critical knowledge, there are a few students with glazed-over expressions that say loud and clear, “Boring!”
Keeping students engaged in learning is an uphill battle, but RT educators have found some great ways to make it happen.
Make learning fun
“We’ve always liked to make learning fun,” said Charity Bowling, MA, RRT, respiratory therapy program director at Ivy Tech Community College in Indianapolis, IN. Games are a big hit with her students.
“One item we like to use in our classroom, especially for review, is the game Kahoot,” Bowling said. “It’s free and the students enjoy it because they use their smartphones, laptops, or even our computers to access it.”
The faster students answer the questions, the more points they earn, and Bowling and her colleagues offer rewards for the top point-getters in the form of small prizes like candy, pens or pencils.
They got the idea from other faculty members on their campus and say it’s worked great to get students engaged.
Code Blue!
Another favorite technique is having someone burst in and interrupt the class with the cry of “Code Blue.” Index cards with a small amount of information about the case are handed out and students must quickly assess the situation, and then form teams to respond.
“We look for leadership, teamwork, evaluation of the steps they are doing, etc.,” says Bowling. “After we are finished, we review what went well and what didn’t go well.”
An individual learning tactic she calls oral exams keeps students on their toes as well. Former graduates act as patients while students interact with them to provide the best care possible based on their signs, symptoms, and other factors.
Students are evaluated on their use of standard precautions, how they interact with the patient, education provided, as well as their communication skills.
“For maximum points, the student must also pick the correct path of treatment,” Bowling said.
Putting it all together
Bowling says her students have responded positively to these activities. While the oral exams can be a bit stressful, they appreciate the chance to identify their strengths and weaknesses, and areas that need improvement.
“We have found in our program the more we can get them moving through group activities, games, etc., the more engaged they are,” Bowling said.
She says pulling it all together has helped students with their critical thinking skills, teamwork, and communication skills.
“We also have seen improvement on test scores in the classroom, and on passing their boards!” Bowling said.
Making sense of the material
Like many RT programs, the one at Boise State University in Boise, ID, includes a cardiopulmonary renal anatomy and physiology course for first year RT students.
“Students who are new to respiratory care get into the course and their heads spin with VD/VT, VCO2, VE, VA, compliance, resistance, and the list goes on,” said Director of Clinical Education Jeff Anderson, MA, RRT, who teaches the course.
And since they won’t actually use the information until they get into their ICU rotations a year later, it’s hard for them to see the value in it.
To help them make sense of the material right now, Anderson decided to bring his students into the ICU so they can see how the physiology information is used.
“We have the luxury of having two full-time faculty paired with four junior students in the ICU, allowing us to reinforce didactic content at clinical,” he explains. “First year students are paired with second year students for two to four six-hour shifts.”
Good feedback
Anderson says the strategy has paid off for first years and second years alike.
“Bringing a first year student into the ICU to observe the second year students using content from their first semester has been a very positive experience for the faculty, the newbies, and the second year students who are able to demonstrate what they have learned,” he said.
He’s received plenty of positive comments.
“The first year students have exclaimed about how eye opening the experience was, and how they might change their study habits to ensure that they grasp the lecture course content for use when they are in the clinical setting,” Anderson said.
Interdisciplinary teaching
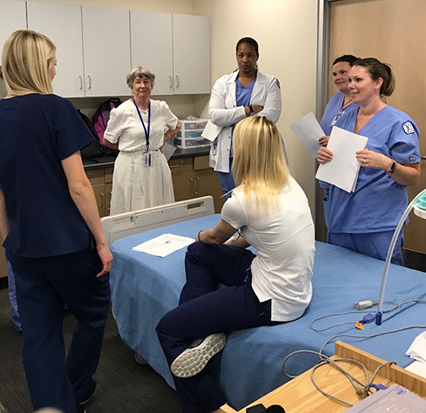
At Illinois Central College in Peoria, Program Director Kelly Crawford-Jones, MS, RRT, has seen great success with an initiative that uses RT students to teach respiratory concepts and skills to nursing students.
“Our freshman students hold a lab for nursing students during their first month of classes,” Crawford-Jones said. “This lab is held at six bedside locations.”
Each student is assigned one of six topics:
- Oxygen and air flowmeters, how to read the meters properly, and safety issues;
- Simple oxygen masks, their sizes, and how to operate them;
- Nasal cannulas, oxygen conserving cannulas, and issues with ear soreness; partial and non-rebreathing masks;
- Venturi masks; and
- Pulse oximetry.
Nursing students receive information handouts and an assessment quiz that follows the training. The students rotate from one bed to the next in groups.
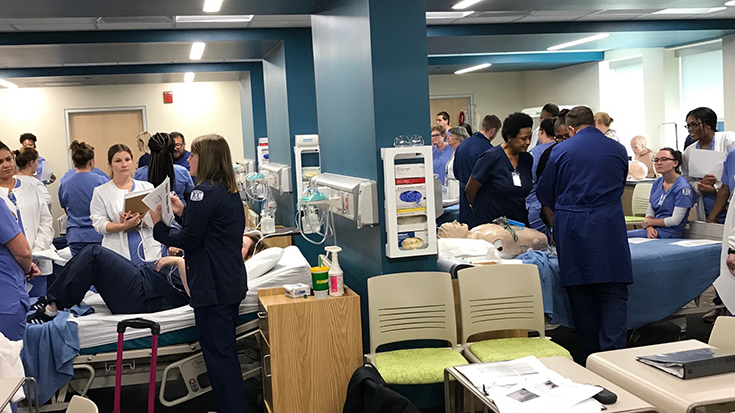
High marks
Crawford-Jones says the lab is always buzzing with excitement during the session and she often gets goosebumps from seeing her RT students do such a great job of imparting knowledge to their colleagues in nursing.
Both RT and nursing students rate the activity highly on evaluations.
“I know that the respiratory therapy students are really pushed to learn this information quickly and thoroughly, but they rise to the occasion,” Crawford-Jones said.
Nursing instructors often ask her if the students are freshmen or sophomores.
“They are amazed at the level of knowledge for new freshmen,” Crawford-Jones said.
Bringing in outside sources
Douglas Masini, EdD, RRT, RRT-ACCS, AE-C, FCCP, FAARC, program director at Armstrong State University in Savannah, GA, has used the VARK quiz to screen new students since the late 1990s and says his students tend to have very strong scores in visual and kinesthetic/psychomotor areas.
They pair these traits with auditory learning and the reading/writing skills needed in respiratory care and bring their clinical affiliates into the mix as well.
“With this information, we added clinical scenarios and outside resources to the classroom and laboratory curriculum,” Dr. Masini said.
For example, seniors are required to take the NIH course on protection of human research participants to make them aware of their responsibilities as researchers and providers, and the program also taps into courses found in AARC University and the AARC collaborative course with Purdue University on tobacco cessation.
“While we have used hands-on high-fidelity simulations in our program for many years, the above components allow another voice to enhance the classroom teaching and learning process,” Dr. Masini said. “It makes faculty acutely aware of the constantly increased expectation of the advanced practice respiratory therapist.”
A great difference maker
Dr. Masini says these resources have made a difference for his students.
“A great example was the final competencies in our advanced ventilation labs, where students were assigned Team Leader or Medical Emergency Team Leader roles in a high-fidelity simulation,” Dr. Masini said.
In addition to being better able to select drugs and calculate dosages, students improved their performance on the psychomotor skills, and also did a better job of information gathering and decision-making, based on what they had learned in their classes and through the ACCS modules.
“I hope to see this knowledge reinforced in their externship experience and translate into their performance on the TMC and CSE,” Dr. Masini said.
For additional ideas on keeping students engaged access AARC’s Student Engagement Book for educators.